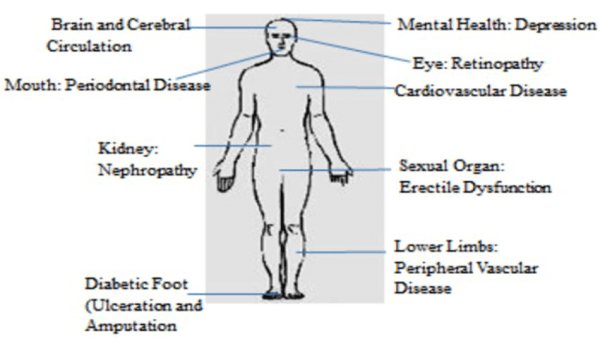
Recap: A plantar wart is a small growth on the foot that is rough in texture and hurts when pinched. It is usually found on the ball of the foot, the heel or the base of the toes. When the wart is paired, black pinpoints are seen in the center. Plantar warts are caused by HPV (Human Papilloma Virus).
Symptoms of Plantar Warts:
-black pinpoints (small clotted blood vessels)
-pain when walking or weight-bearing
-rough callus can form on top of the wart (this is where a wart has grown inward)
Plantar warts may disappear without treatment. Otherwise, you can ask your doctor for treatment. Another option is to see a podiatrist or a chiropodist. A foot care nurse can also help.
Prevention
-make sure to use different foot care instruments and supplies for the wart than for healthy skin and nails
-don’t scratch the wart with your nails. Wash your hands after touching it.
-wear sandals in the pool area and slippers in the house
-keep feet clean and dry through daily hygiene
Tell your doctor if:
-you also have Neuropathy and/or Diabetes
-the wart has been treated but it persists, recurs, and/or multiplies
-the growth has changed in colour or shape, is painful and/or bleeding
-the pain is affecting your activities of daily living
-you’re not sure if the growth is a wart
-you have a weak immune system
Possible treatments:
-your family doctor, podiatrist, or chiropodist may use 50% Salysilyc Acid or Nitrous Oxide
-the health care provider will pinch the area where the wart was in 2 places and say “here is 1 (pinch), here is 2 (pinch), does one and two feel the same?” If there is sharp pain, that means the wart is still there just not visibly.
-over the counter solutions you can use at home include Compound W (use nightly by applying on the wart with applicator or Q-tip) or Canthacur (Cantharidin 0.7%)
-cover with Opsite Flexfix and then Hypafix tape after application of solution.The tape used has to be waterproof and can be bought in a pharmacy. Keep covered so that no air gets in. Leave on when showering.
-after treatment application at home you still have to see a podiatrist, chirpodist or a specially trained foot care nurse for conservative debridement.